Since sperm cannot leave the body after a vasectomy, many men are left wondering–where does the sperm go? The simple answer is that the body will reabsorb the sperm. But how exactly does this process work?
Sperm reabsorption is not something that occurs solely with vasectomized men. All men produce millions of sperm that do not make it to ejaculation and are reabsorbed into the body. Sperm within the testicle are immature and cannot fertilize an egg–they mature in the epididymis.
How does sperm reabsorption work normally?
Sperm are moved from the seminiferous tubules within the testicular structure to the epididymis for maturing and storing. They stay in the epididymis for about a month, and at the end of this time are either degenerated and absorbed, or are expelled to begin the journey up the vas deferens to the ampulla for storage prior to ejaculation. Animal studies estimate that 40%–50% of sperm produced are reabsorbed before they reach the vas deferens.1Alexander N. Vasectomy: long-term effects in the rhesus monkey. J Reprod Fertil. 1972;31(3):399-406. doi:10.1530/jrf.0.0310399
When some obstruction to sperm exiting the epididymis occurs, a “compensatory action” happens to avoid permanent testicular dysfunction. Obstruction does not necessarily mean vasectomy–various medical conditions may cause temporary or permanent obstruction.
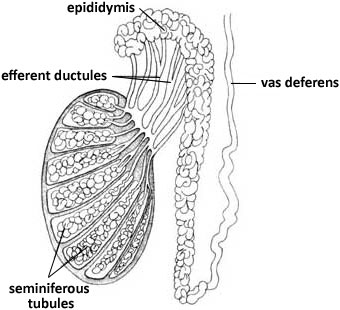
Epididymis
As illustrated in the diagrams, the epididymis is an extensively coiled tubular organ attached to the posterior surface of the testis. If you uncoiled it, you would end up with one tube about 5-6 m (about 17 ft) long!2Quah S. International Encyclopedia Of Public Health. Oxford: Academic Press; 2017.
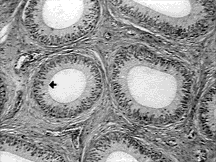
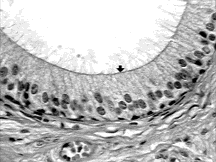
Cross Section A and Cross Section B are of the epididymis. Although the pictures give the impression you are looking at several epididymal ducts, what you see a cross-section of one highly convoluted duct. Cross Section B is a magnification of Cross Section A. The duct is lined with tall columnar epithelium with prominent Stereocilia.
Columnar Epithelium
A sheet-like lining entirely devoid of blood vessels, but rich in nerve endings. In the epididymis, the epithelium is “columnar”. This means it’s not a flat surface, but highly textured and looks a little like the texture or a brush under magnification. This dramatically increases the surface area available. Cross-section 2 shows the brush-like texture of the inner surface of the duct.
Stereocilia
The stereocilia are actually extremely long microvilli (finger-like extensions) covering the free surface of the epithelial cells. As in the columnar structure of the epithelium, this allows a tremendous increase in the surface area of the cell for absorption or secretion. Stereocilia are not able to move in the powerful manner characteristic of true cilia. ‘Stereo-‘ means firmly attached or in other words non-motile. They occur only in two places – here in the epididymal duct, and in the inner ear.
What changes after a vasectomy?
Post-vasectomy, the diameter of the ducts increases 2 to 4 times their original size to counteract the increase in fluid pressure,3Jarow J, Budin R, Dym M, Zirkin B, Noren S, Marshall F. Quantitative pathologic changes in the human testis after vasectomy. A controlled study. N Engl J Med. 1985;313(20):1252-1256. doi:10.1056/NEJM198511143132003 and fluid absorption is increased, particularly in the efferent ducts, where 90% of excess fluid is reabsorbed.4Nistal M, Riestra M, Galmés-Belmonte I, Paniagua R. Testicular biopsy in patients with obstructive azoospermia. Am J Surg Pathol. 1999;23(12):1546-1554. doi:10.1097/00000478-199912000-00013 The level of macrophages will increase within the epididymis. Macrophage means “big eater”. Macrophages are white blood cells that crawl around in the extracellular fluids of your body and gobble up microbes, other foreign material, and natural cellular debris. They ingest these microbes and debris by phagocytosis (“cell eating”). Parts of the cell surround the particle to be eaten, then the macrophage’s membrane flows together and the particle ends up inside where chemicals and enzymes break down the molecules into their basic components.
3 months after vasectomy the number of macrophages laden with phagocytized sperm will drastically increase throughout the epididymis.5Linnet L. Clinical immunology of vasectomy and vasovasostomy. Urology. 1983;22(2):101-114. doi:10.1016/0090-4295(83)90487-9 The task of reabsorbing the sperm over-whelms the epithelial cells (the usual method of reabsorption) and more macrophages are recruited from the circulation to aid in their digestion and clearance.
Summary
After a vasectomy, sperm can’t get into semen and leave the body through the penis. Sperm will still be produced by the testicles but is dissolved and naturally absorbed by the body. Most of the fluids are absorbed in the epididymis by membranes. Most of the solid matter is broken down by macrophages and reabsorbed through the bloodstream.
After the procedure, the membranes will expand to absorb and store the extra fluid, which also causes the immune system to deliver additional macrophages to break down and reabsorb more of the solid content.
References and further reading
Vasectomy-Information.com has a strict sourcing policy. We rely on evidence-based medicine, peer-reviewed studies, reputable clinical journals, and medical associations. Learn more about how we ensure our content is accurate and up-to-date by reading our editorial policy.- Alexander N. Vasectomy: long-term effects in the rhesus monkey. J Reprod Fertil. 1972;31(3):399-406. doi:10.1530/jrf.0.0310399
- Quah S. International Encyclopedia Of Public Health. Oxford: Academic Press; 2017.
- Jarow J, Budin R, Dym M, Zirkin B, Noren S, Marshall F. Quantitative pathologic changes in the human testis after vasectomy. A controlled study. N Engl J Med. 1985;313(20):1252-1256. doi:10.1056/NEJM198511143132003
- Nistal M, Riestra M, Galmés-Belmonte I, Paniagua R. Testicular biopsy in patients with obstructive azoospermia. Am J Surg Pathol. 1999;23(12):1546-1554. doi:10.1097/00000478-199912000-00013
- Linnet L. Clinical immunology of vasectomy and vasovasostomy. Urology. 1983;22(2):101-114. doi:10.1016/0090-4295(83)90487-9
- Christiansen CG, Sandlow JI. Testicular Pain Following Vasectomy: A Review of Postvasectomy Pain Syndrome. Journal of Andrology. Published online May 6, 2003:293-298. doi:10.1002/j.1939-4640.2003.tb02675.x